Head and face reconstruction
Definition
Head and face reconstruction is surgery to repair or reshape deformities of the head and face (craniofacial surgery).
Alternative Names
Craniofacial reconstruction; Orbital-craniofacial surgery; Facial reconstruction
Description
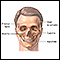
How surgery for head and face deformities (craniofacial reconstruction) is done depends on the type and severity of deformity, and the person's condition. The medical term for this surgery is craniofacial reconstruction.
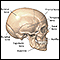
Surgical repairs involve the skull (cranium), brain, nerves, eyes, and the bones and skin of the face. That is why sometimes a plastic surgeon (for skin and face) and a neurosurgeon (brain and nerves) work together. Head and neck surgeons and maxillofacial surgeons also perform craniofacial reconstruction operations.
The surgery is done while you are deep asleep and pain-free (under general anesthesia). The surgery may take 4 to 12 hours or more. Some of the bones of the face are cut and moved. During the surgery, tissues are moved and blood vessels and nerves are reconnected using microscopic surgery techniques.
Pieces of bone (bone grafts) may be taken from the pelvis, ribs, or skull to fill in spaces where bones of the face and head were moved. Small screws and plates made of titanium or a fixation device made of absorbable material may be used to hold the bones in place. Implants may also be used to help reshape the skull. The jaws may be wired together to hold the new bone positions in place. To cover the holes, flaps of tissue may be taken from the hand, buttocks, chest wall, or thigh.
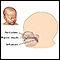
Sometimes the surgery causes swelling of the face, mouth, or neck, which may last for weeks to months. This can block the airway. For this reason, you may need to have a temporary tracheostomy. This is a small hole that is made in your neck through which a tube (endotracheal tube) is placed in the airway (trachea). This allows you to breathe when your face and upper airway are swollen.
Why the Procedure Is Performed
Craniofacial reconstruction may be done if there are:
- Birth defects and deformities from conditions such as cleft lip or palate, craniosynostosis, Apert syndrome
- Deformities caused by surgery done to treat tumors
- Injuries to the head, face, or jaw
- Tumors that have been removed
Risks
Risks of anesthesia and surgery in general are:
- Problems breathing
- Reactions to medicines
- Bleeding, blood clots, infection
Risks of surgery of the head and face are:
- Nerve (cranial nerve dysfunction) or brain damage
- Need for follow-up surgery, especially in growing children
- Partial or total loss of bone grafts
- Permanent scarring
These complications are more common in people who:
- Smoke
- Have poor nutrition
- Have other medical conditions, such as lupus
- Have poor blood circulation
- Have past nerve damage
After the Procedure
You may spend the first 2 days after surgery in the intensive care unit. If you do not have a complication, you will usually be able to leave the hospital usually within 1 week. More limited procedures may require shorter or no hospital stay. Complete healing may take 6 weeks or more. Swelling will improve over the following months.
Outlook (Prognosis)
A much more normal appearance can be expected after surgery. Some people need to have follow-up procedures during the next 1 to 4 years.
It is important not to play contact sports for 2 to 6 months after surgery or until your surgeon says it is OK.
People who have had a serious injury often need to work through the emotional issues of the trauma and the change in their appearance. Children and adults who have had a serious injury may have post-traumatic stress disorder, depression, and anxiety disorders. Talking to a mental health professional or joining a support group can be helpful.
Parents of children with deformities of the face often feel guilty or ashamed, especially when the deformities are due to a genetic condition. As children grow and become aware of their appearance, emotional symptoms may develop or get worse.
References
Baker SR. Reconstruction of facial defects. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head & Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 21.
Padilla PL, Khoo KH, Ho T, Cole EL, Sirvent RZ, Philips LG. Plastic surgery. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery: The Biological Basis of Modern Surgical Practice. 21st ed. St Louis, MO: Elsevier; 2022:chap 69.
Review Date:5/6/2025
Reviewed By:Tang Ho, MD, Associate Professor, Division of Facial Plastic and Reconstructive Surgery, Department of Otolaryngology – Head and Neck Surgery, The University of Texas Medical School at Houston, Houston, TX. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
The information provided herein should not be used during any medical emergency or for the diagnosis or treatment of any medical condition. A licensed medical professional should be consulted for diagnosis and treatment of any and all medical conditions. Call 911 for all medical emergencies. Links to other sites are provided for information only -- they do not constitute endorsements of those other sites. © 1997-A.D.A.M., Inc. Any duplication or distribution of the information contained herein is strictly prohibited.
The Agency for Health Care Administration (Agency) and this website do not claim the information on, or referred to by, this site is error free. This site may include links to websites of other government agencies or private groups. Our Agency and this website do not control such sites and are not responsible for their content. Reference to or links to any other group, product, service, or information does not mean our Agency or this website approves of that group, product, service, or information.
Additionally, while health information provided through this website may be a valuable resource for the public, it is not designed to offer medical advice. Talk with your doctor about medical care questions you may have.